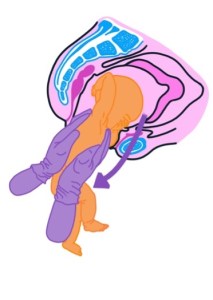
Vaginal breech birth (VBB) is a controversial area of research, in an area of high obstetric litigation. Understandably, people are wary of introducing changes in practice that could expose them, mothers or babies to additional risks. Our research team responds frequently to questions and challenges about our approach, how it aligns with national guidance, and the evidence base.
Recently, a colleague became concerned after reading that the Health Services Investigation Board (HSIB) had presented evidence in Parliament in 2020 about the use of an algorithm to assist a baby’s birth.

The report did not indicate which algorithm was used in this instance, and there are many in circulation. Neither Breech Birth Network nor the OptiBreech Collaborative have ever produced an algorithm for use by maternity triage teams to support breech births at home, nor have we ever promoted the use of our algorithm for this purpose. We have not been informed by any sites in the south-east of England that have been using our algorithm that they have been instructed by the HSIB to stop using it.
How does the OptiBreech Algorithm align with national guidance?
The Physiological Breech Birth Algorithm (OptiBreech Algorithm) is designed to guide clinical decision-making during simulation training, to develop these skills for use in practice. The Vaginal Breech Birth training is delivered via the Royal College of Obstetricians and Gynaecologists (RCOG). The 2023 course was attended by 105 obstetricians and midwives from across the UK, and international visitors.
The description of manoeuvres in our algorithm is fully compliant with RCOG Management of Breech Presentation guidance, which states that, “If the operator has the skills of undertaking the manoeuvres with the mother in a forward position these should be performed without delay.”
In the RCOG guideline, all evidence relating to management of active second stage is based on ‘expert opinion.’ This guidance states that, “[I]ntervention to expediate breech birth is required if there is evidence of poor fetal condition or if there is a delay of more than 5 minutes from delivery of the buttocks to the head, or of more than 3 minutes from the umbilicus to the head.”
How does the OptiBreech Algorithm differ from national guidance?
Our Algorithm and OptiBreech guideline recommend that the birth should be complete within (including time for manoeuvres): 7 minutes from rumping (both buttocks and anus visible on the perineum), 5 minutes from the birth of the pelvis, and/or 3 minutes from the birth of the umbilicus. This is more conservative than the RCOG guideline and, in principle, less likely to contribute to delay in a baby’s birth – unless earlier intervention actually causes complications (see below).
The RCOG guidance was published in 2017 and is intended to be updated every three years. It has not since been updated, but that does not mean that the evidence base has not moved on.
What evidence is the OptiBreech Algorithm based on?
First version
The first version of the Physiological Breech Birth Algorithm was used in Breech Birth Network training in 2017. It was based on video evidence conducted with Dr Anke Reitter. This structured study of video evidence measured median and range interval times for a series of upright breech birth videos. We also recorded the observable mechanisms (position changes) of the breech baby as they journeyed out of the maternal pelvis, and how these related to whether attendants used interventions to facilitate the birth. From this data, we produced an algorithm, including indications that assistance is needed and which interventions were indicated.
Prior to this, training had been based on a combination of instructing attendants to remain “Hands off the breech,” or to perform a set of routine manoeuvres, each of which are only appropriate to supine positions. This was clearly causing confusion and delay.
Refinements
Midwife Emma Spillane then further tested the time intervals with a case-control design and found similar results. While head and arm entrapment only occurred once each, when interventions were used, attendants to ‘case’ births (neonatal admissions or death) waited almost twice as long to intervene as those at ‘control’ births (no neonatal admission).
How has the OptiBreech Algorithm been tested in practice?
Currently, the OptiBreech Algorithm guides vaginal breech birth management within all OptiBreech research, alongside a more detailed OptiBreech Practice Guideline. These materials are reviewed regularly within the OptiBreech Collaborative, based on reviews of their use in practice and our continually evolving evidence base. We follow a Community of Practice approach and host frequent webinars focused on developments in practice.
There are more outcome data associated with use of the OptiBreech Algorithm than any other breech algorithm we can identify. To date, we have evaluated the effects of training and service delivery based on the OptiBreech Algorithm in three prospective studies:
In our 2016-2019 evaluation, obstetricians and midwives received training in ‘physiological breech birth’ based on the OptiBreech Algorithm. We compared clinical outcomes for births attended by someone who had completed the training with those not attended by someone who had completed the training. We prospectively recorded 0/21 (0%) severe neonatal outcomes when VBBs were attended by someone who had completed the OptiBreech training, compared to 5/69 (7.2%) where no clinicians present had completed the training.
We evaluated how well thirteen National Health Service (NHS) hospitals were able to implement breech intrapartum teams and provide OptiBreech-trained professionals for VBBs, planned or unplanned. This study observed one neonatal SAE among 82 planned (1.2%) and 40 actual VBBs (2.5%). In the birth where the SAE occurred, the woman was positioned in a supine position, had spinal anaesthesia prior to the start of second stage, and Loveset’s and Mauriceau-Smellie-Veit (M-S-V) were used as instructed in the PROMPT flowchart.
Among VBBs, 34/39 (87.2%) were complete within 5 minutes of the birth of the pelvis. One was born very quickly, without an attendant, so the data is missing.
The prospective observational cohort (In Press)
Our prospective observational cohort study collects outcomes for women who receive OptiBreech collaborative care for a planned or unplanned VBB, currently across 10 NHS sites. Management of labour is based on the OptiBreech Algorithm and Practice Guideline.
In our latest analysis of data received to 8 September 2023, the database records 97 planned and 42 actual VBBs. None of them involved a neonatal SAE. Two babies had an Apgar <7 at 5 minutes (2.1%). We have interval data available for 30 of these births, and 27 of them (90%) were completed within 5 minutes of the birth of the pelvis.
Total prospective VBBs
These studies include a total of 200 prospectively observed* and 103 actual OptiBreech VBBs, with one neonatal SAE. This corresponds to a rate of 0.5% for planned VBB and 1.0% for actual VBBs to date.
(* The training evaluation did not include planned VBBs that ended in caesarean birth. These rates could change as we accumulate further data.)
How does this compare to other vaginal breech birth research?
To measure neonatal severe adverse events (SAEs), we use a composite measure, that is made up of: neonatal mortality (death, neonatal admission to SCBU/NICU for >4 days, Apgar <4 at 5 minutes, HIE Grade 3, Intubation / ventilation >24 hours, parenteral or tube feeding >24 hours, seizures or convulsions > 24 hours, peripheral nerve / brachial plexus injury present at discharge, skull fracture, spinal cord injury). This measure is based on a similar composite used in the Term Breech Trial and PREMODA studies.
In the Term Breech Trial, the neonatal SAE rate for planned VBB was 52/1039 (5.0%) overall and 29/511 (5.7%) in countries with a low overall perinatal mortality rate, such as the UK.
In PREMODA, the neonatal SAE rate for planned VBB was 40/2502 (1.6%).
In the largest study of VBB in the UK this century, Pradhan et al reported a low Apgar (<7 at 5 minutes) rate of 52/882 (5.9%).
Does immediate assistance result in more complications?
Among the 103 actual VBBs we have evaluated, 88.4% were completed within five minutes of the birth of the pelvis, and the neonatal SAE rate was 1%. A rate of 88.4% under 5 minutes is NOT achievable without actively encouraging or assisting the birth. Our guidance is clearly not resulting in an increase in serious complications. In our next analysis, we will look at rates of assistance and minor complications.
Who are the OptiBreech Collaborative? And what is the basis for their claims of expertise?
The OptiBreech Collaborative consists of the Principal Investigators for our research at various sites across the UK, including breech specialist midwives and obstetricians. We all support planned (and unplanned), term, singleton VBBs regularly. Names are acknowledged in our recent publications. The Collaborative is led by Dr Shawn Walker, a consultant midwife and the chief investigator of the OptiBreech studies.
The RCOG guidance states, “Guidance for the case selection and management of vaginal breech birth should be developed in each department by the healthcare professionals who supervise such births.”
You would be hard pressed to identify a lead obstetrician in the UK who has clinically led a team that has supported 200 planned, term, singleton VBBs over the past six years. That is essentially what we have done — during a pandemic, in severely stretched NHS hospitals, without the backup of clear national guidance, and often in the face of extraordinary resistance to our efforts.
We are not even certain the authors of the RCOG guidance, who are eminent, experienced and well-respected obstetricians, are regularly supervising planned, term, singleton VBBs. We certainly know that a majority of consultant obstetricians in the UK are not regularly supervising planned, term, singleton VBBs. If women are to be believed, many professionals are actively discouraging planned VBB by providing only inaccurate and/or biased information.
The RCOG guidance points to ‘an article by Evans’ (not publicly available) to describe the technique and manoeuvres to be used for VBBs in an ‘all fours’ position. We absolutely credit Jane Evans and Mary Cronk with introducing VBB in an ‘all fours’ position to UK practice with the first ever training provided, and their training was our starting point. Mary Cronk (who attended a total of 25 VBBs in her career) introduced the phrase, “Hands off the breech.” This has been widely adopted by the RCOG and other guidelines. But neither Evans nor Cronk has ever shared any outcome data. The OptiBreech effort has transparently reported 200 prospectively observed VBBs.
While we eagerly began with Evans-Cronk methods, our own experience and research has simply taught us that we get better outcomes when we assist the birth sooner rather than later, using our physiology-based, responsive approach rather than a routine set of manoeuvres. That is what we practice, that is what we evaluate, and that is what we teach.
We never expected that we would end up recommending more active intervention and liberal use of episiotomy with any delay on the perineum (after other methods are used). But there is no point in doing research if you do not believe the results and allow it to guide your practice.
What is the evidence for other algorithms currently in use?
We cannot identify a single study that has compared outcomes for VBBs before and after training based on a different breech algorithm with actual clinical outcome data that improved, other than ours.
We have identified one study (Hardy et al 2020), which evaluated training based on the ‘appropriate manoeuvres,’ Lovesets and M-S-V. The pre-training low Apgar rate was 0/56 and post-training it was 7/80 (8.8%, p=0.041). Special care nursery admissions also increased. In our view, these methods should not continue to be taught unless someone can produce any evidence at all that teaching them improves clinical outcomes.
In 2021, we escalated our concerns to the then President of the RCOG and the Chief Executive of the RCM, who have promised us a review of current guidance. We hope, for the sake of breech babies and their parents, that this review begins soon.
We would be happy to be corrected. Please do direct us to any available empirical evidence underpinning other breech training or algorithms currently in use across the UK or elsewhere.
— Shawn