Dr Shawn Walker, Consultant Midwife and Chief Investigator, explains the OptiBreech position on planned vaginal breech birth at home.
OptiBreech position on home breech birth — The OptiBreech Project


Dr Shawn Walker, Consultant Midwife and Chief Investigator, explains the OptiBreech position on planned vaginal breech birth at home.
OptiBreech position on home breech birth — The OptiBreech Project

Update December 2023: We are pleased to announce that our fully-evaluated course, the foundational training for those participating in the OptiBreech Trial, will be offered for the second year in a row through the Royal College of Obstetricians and Gynaecologists, on 9 May 2024 — Book here.
This will be of particular interest to obstetric specialty trainees, many of whom will be able to use study leave and have course fees paid (50%) through educational budgets because the course is hosted by the RCOG.
We look forward to supporting more obstetricians, midwives and paramedics to feel confident in their ability to support vaginal breech births, and to provide appropriate hands-on assistance when indicated.
Spaces limited. Book here.

This Monday, we held a training day at St. Mary’s Hospital in Paddington, London, to support the Imperial OptiBreech Team, led by Consultant Obstetrician Sabrina Das.
We will be donating 10% of any revenue obtained from this and all future study days to the OptiBreech Just Giving page, which is raising money to provide sites with extra support so that team members can continue to be on-call for women planning a vaginal breech birth.
We would be incredibly grateful if you would join us in this support by donating if you can and sharing the link with your social networks.
Below is some recent research to demonstrate how we are helping to make breech services better and safer for all families:
First OptiBreech results poster! Walker, S., Dasgupta, T., Hunter, S., Reid, S., Shennan, A., Sandall, J., Davies, S., 2022. Preparing for the OptiBreech Trial: a mixed methods implementation and feasibility study. BJOG An Int. J. Obstet. Gynaecol. 129, 70. https://epostersonline.com/rcog2022/node/4909
Spillane E, Walker S, McCourt C, 2022. Optimal time intervals for vaginal breech births: a case-control study. NIHR Open Res. 2, 45.https://doi.org/10.3310/nihropenres.13297.1
Walker S, Dasgupta T, Halliday A, Reitter A, 2021. Development of a core outcome set for effectiveness studies of breech birth at term (Breech-COS): A systematic review on variations in outcome reporting. Eur. J. Obstet. Gynecol. Reprod. Biol. 263, 117–126. https://doi.org/10.1016/j.ejogrb.2021.06.021
Yesterday was International Day of the Midwife. I saw but didn’t participate in the social media celebrations. Not because I wasn’t feeling it, but because my clinical academic midwife life was full to the brim. This included:

If you feel exhausted just reading that list, you’re as human as me!
A team is not a group of people that work together. A team is a group of people that trust each other.
– Simon Sinek, shared by Céline, an attendee at my VIDM presentation
This feasibility study is undoubtedly the most challenging and most rewarding thing I have ever done in my life. Being a research leader means being a change leader, and change is never easy. The OptiBreech Project is proposing a paradigm change in the way we support vaginal breech birth. This means a change from promoting caesarean section (CS) to supporting each individual women’s choice of mode of birth, in line with NICE Guidance. And it means a change from using unreliable ‘selection criteria,’ which are also inconsistent with the concept of individual choice, to relying on specialist expertise to respond to unfolding and infinitely unique circumstances.

Being a breech specialist is not easy. In addition to a lot of time spent on-call, it’s not like working in a low-risk midwifery setting, where you can anticipate 90% of women will have the normal birth that they want. Many women are heart-broken when they find out their baby is breech. We can support them to plan an elective CS, and some women are happy about this, but many are very disappointed, even when they feel this is the best option for them and their baby. For those who want to plan a vaginal birth, but only if the baby is head-down, baby turning (ECV, external cephalic version) is only successful up to 50% of the time. We are still there for women when it does not work.
For those who want to plan a vaginal breech birth, the barriers sometimes seem impossible. It’s not uncommon for women to make an informed decision to plan a physiological breech birth (PBB) and return to clinic in tears because of the way someone has spoken to them, be that another health care professional, a friend or family member, or an unkind stranger on social media with opinions about the wisdom of their choice. The criticism, judgement and stigma can feel very heavy at such a vulnerable time. Our interviews with women on the study indicate they have felt supported to change their minds and plan an elective CS in these circumstances. Of course we can and do facilitate women changing their minds, but we can’t take away the hurt women feel when they wished for more support to make a different choice.
Birthing people who stick with their choice to birth vaginally despite such ubiquitous doubt frequently want reassurance that everything will be okay. Of course, we can never guarantee a perfect outcome. We can only guarantee that we are doing our best to increase the chances we will get professionals with enhanced training and experience to their birth. We believe this will improve outcomes for these births (that is the premise of the research), but we will not know until many OptiBreech births have occurred. And we all have to be prepared for a higher need for intrapartum CS to achieve a safe outcome for breech babies, even when trying for a vaginal birth.
Those of us supporting women who choose physiological breech births face similar criticism and judgement on a regular basis. Sometimes the lack of respect and unkindness feels overwhelming, and it is tempting to succumb to despair. I find it helps to remember that behaviour like this comes from a place of fear, a belief that doing things differently could have disastrous outcomes. Nobody wants this, and nobody wants to be responsible for it. In difficult times, I lean into the support I feel from many wonderful midwifery and obstetric colleagues, who help bring me back to a place of compassionate understanding. Only by opening to understanding each other can we move towards trust and safety — physical, emotional and spiritual safety in each others’ hands.
Listening to my ‘Joy and Love’ playlist helps too. Here’s a mini playlist of my favourite Resistance Revival Chorus songs, for anyone who needs them today.

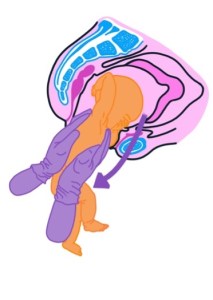
Shawn Walker, RM PhD, King’s College London and Chelsea and Westminster Hospital NHS Foundation Trust, West Middlesex Hospital Sabrina Das, MB ChB, MRCOG, Imperial College Healthcare NHS Foundation Trust, Queen Charlottes & Chelsea Hospital Emma Spillane, RM MSc, Kingston Hospital NHS Foundation Trust Amy Meadowcroft, RM, Northern Care Alliance NHS Foundation Trust Background In the […]Continuous cyclic pushing: a non-invasive approach to optimising descent in vaginal breech births — The OptiBreech Project

The recent release of the final Ockenden Report has shed light on deeply painful experiences for the women, families and healthcare professionals involved. For those of us who have not been involved, the call to deep reflection can also be a painful experience, but a necessary one.
I have been asked by several people what I feel this means for vaginal breech birth. Will women still want one after this report, where promotion of vaginal breech birth against maternal request for a caesarean section was a contributing factor in some very sad outcomes? Will professionals be even more reluctant to support women who wish to choose a vaginal breech birth, for fear of being accused of zealous pursuit of normal birth at all costs?
My answer is this: I welcome this report because I see it as affirmation of the need for individualised care, the need to listen to women, the need to place their values and needs at the centre of care.
Women who want a caesarean section, regardless of their baby’s presentation, should have easy access to one. I counsel several women with a breech-presenting baby every week about their birth choices, and I encounter many women who appear to be somewhat relieved that their baby is breech. They do not want an attempt at baby turning (external cephalic version, ECV, to a head-down position). They want a caesarean section. And their baby being breech means they will have one without the need to justify their choice.
I stopped talking women into an attempt at baby turning (ECV) a decade ago because I audited the results of my first breech clinic. By introducing a breech specialist midwife pathway, I doubled the rate of ECV acceptance almost overnight. Women trusted me. For two women, I remember clearly convincing them that ECV was ‘best.’ I even said to one after a successful procedure, “Aren’t you glad you had a go?” One woman had a long, complicated induction that ended with an emergency caesarean section and massive obstetric haemorrhage (bleeding). The other had a failed attempt at suction cup delivery, failed attempt at forceps delivery and a caesarean section. I have also been present when an ECV attempt at 36 weeks led to an emergency caesarean section, in which we found the cord ended up in front of the baby’s head as it was trying to engage. I’m pretty sure none of these women ended up happy that someone convinced them to have an ECV rather than a planned CS. If this has been your experience, or similar, I am so deeply sorry.
But I also meet many women who decide that an attempt at baby turning is the best choice for them. They really want to try for what they see as a ‘normal birth,’ in a birth centre with midwives and access to the birth pool. They are prepared to accept the relatively small risks associated with ECV and vaginal birth — after all, I can remember these women as individuals after a decade of doing breech work — because they feel the potential benefits outweigh the risks. These women deserve to be offered this attempt, with experienced providers who have a consistently good success rate. And if adverse outcomes happen, they deserve NOT to be treated as if they made the wrong decision. None of us has a crystal ball.
It is my responsibility to explain why baby turning is the nationally recommended ‘treatment’ for breech presentation. When I explain this, I explain the potential benefits of and increased likelihood of having a straightforward vaginal birth, particularly in a first pregnancy. I also explain to every woman that, in 2022, by far the most likely outcome no matter what she chooses to do (ECV, VBB, CS) is that she and her baby will be well and safe following the birth. There are small differences in risk between each choice, but ultimately, with skilled support and a plan in place, the outcomes are very good for all choices. She should feel supported to make the choice that ‘feels’ right to her. We professionals should then do our best to make this choice as safe as possible, while continuing to communicate any changes to the risk profile she initially accepted.
I deeply feel that women who want a caesarean section should be able to have one, without judgement or difficulty. I am reassured by our qualitative data in the OptiBreech study, that the breech specialist midwives and breech clinic obstetricians providing counselling are all doing it in a way where women feel they have genuine choices but are not pressured in one direction in another. Participants say this repeatedly and express how much they value this balanced counselling.
I also deeply feel that women who want to attempt a physiological breech birth should have the best possible support for that option. They should also feel their choice is supported without judgement, shame or pressure. Part of enabling women to make this choice involves enabling healthcare professionals to develop skills and work in ways that make ‘a vaginal breech birth with skilled and experienced support’ – which the RCOG guideline tells us should be nearly as safe as a cephalic birth – possible. This is a win-win situation. By supporting the women who WANT to plan a physiological breech birth well, we also increase our skill level to support those rare occasions when there is no choice available due to the rapid progress of an early or unplanned breech labour. When this occurs in the context of rigorously governed research, we can be even more confident that this learning will occur.
Sadly, this is not possible for most women in the UK. Every meeting of our OptiBreech Patient and Public Involvement (PPI) group involves talking through some amount of trauma. Our research team includes women who have sadly lost their babies to poor care and want to preserve the choice with BETTER care and women who have experienced severe complications from caesarean sections they did not want. But almost ALL members of our group, including partners, have expressed trauma from being repeatedly blocked, judged and unable to access skilled, supportive care for a vaginal breech birth. They have read national guidelines that said this should be an option, then found that their local health services had zero commitment to delivering this; they effectively had no choice.
On the other hand, our PPI group has been adamant that they do not want research to demonstrate vaginal breech birth is BEST. They want research to demonstrate what the actual, current risks are for all choices, and to show us how we can help all women make the choice that is right for them.
The vaginal breech birth skill set has remained largely static since the 1970’s, with ‘put the woman in an upright position’ being virtually the only innovation in breech care – until recently. It is as if we have been managing shoulder dystocia with only McRoberts and Gaskin manoeuvres – of course we would expect bad outcomes. (shoulder dystocia = where the baby’s shoulders become stuck in a head-first birth; McRoberts = pulling the woman’s legs back to her abdomen to create space in the pelvis; Gaskin = turning the woman to a hands/knees position)
Yet many professionals trying very hard to do the research we need to improve outcomes for breech babies are also exposed to the trauma of incivility and lack of respect. There is a particular power dynamic that exists between obstetricians and midwives that can make uncooperative behaviour threatening and dangerous – because the best outcomes for planned vaginal breech births are achieved when there are skilled, trusted care providers and a low threshold for using interventions (such as caesarean section) when they are needed. If you are afraid to refer to a person who has previously spoken to you harshly, publicly criticised you or outright refused to have anything to do with a physiological breech birth, this can introduce hesitation where there should be none. Some midwives have also found it difficult to maintain engagement with some women because being called to repeatedly justify women’s choices to colleagues is very emotionally draining, leading to avoidance behaviour. This is neither healthy, nor safe.
Multiple obstetricians who have tried to progress OptiBreech research have also experienced blocking, incivility, and general lack of respect. Discussions have been shut down before they begin. Junior doctors who want to learn the skills find they have no support to do this and remain silent. This has led to communication breakdowns and undermined safety at a time when we all need to be working at our best to learn and improve.
Do I think there is a place for physiological breech birth post-Ockenden? The demand for skilled breech care continues, and we are contacted each week from across the UK by women who are looking for support. In our OptiBreech project, there have been exemplars of healthy communication and excellent teamwork to achieve good outcomes for mothers and babies, and we are focusing on these as the way forward. I am grateful for the warm and respectful interactions I have with many of my colleagues; these sustain us all in our challenging everyday work. Examples of successful co-operation are especially valuable given the extreme pressures staff have been facing with chronic under-staffing and pandemic conditions. And our learning about how to support breech births well is accelerating at light speed as we share our experiences through constant reflection among OptiBreech leads at active sites. We will persist for as long as we can.
Enabling physiological breech birth, and research about how to make it safer, is NOT about promoting natural birth at all costs, nor about promoting natural birth at all. It is about placing the women who use our services at the centre of all we do, bringing our best to meet them where they are at and constantly striving for better. Which is, in my opinion, what the Ockenden Report calls us to do.
This blog is the personal opinion of Dr Shawn Walker and not the NIHR, King’s College London or any NHS institution.
We are thrilled that so many practitioners around the world are using our online resources to share the skills and learning with others in their organisations. We cannot keep up with requests for the new password, which is a wonderful problem to have. 😊
The password for our Physiological Breech Birth video library on Vimeo changes at the beginning of each year. This is for two reasons:
First, to offer some measure of protection from circulation without permission. We are incredibly grateful to the women, families and healthcare professionals who have allowed us to use their videos.
Second, we need to be able to financially support these platforms. So the password continues to be available for anyone who has purchased and has access to our online training platform or the refresher course. To access the refresher course, you first need to complete the main course. Read more.
To access the video library:



Happy new year, breech advocates! We’ve got nearly 10 hours of evidence-packed, video-rich, detail-loving breech birth training content waiting for you.
Our fully updated 2022 course is now on-line. To help you reach your new year’s resolution of developing some beautiful breech skills, the course will be available at a discounted price of £50 for the first two weeks of January. No code needed; access is for one year.

Along with a new course, our Vimeo library has a NEW PASSWORD. This is available from the “Resources for Teaching and Implementation” section of any course you are enrolled in, along with our amazing Dropbox of guidelines and training resources. Registered users have permission to use the content for non-profit teaching purposes — because learning together is the safest, most effective way to do it.
More about why we change this on an annual basis.
All of our online courses also come with free access to our Online Webinars. These are one-hour discussions on topics that have arisen during the course of our practice or others’, where we share learning and reflection with each other.
If you have previously completed any of our on-line courses, you are eligible to register for the Refresher course for only £10/year. This is exactly the same as the main course, but for a nominal cost to help us keep our platforms online. You can review the course, or just complete the assessment to obtain a new certificate for your portfolio.
Anyone organising or attending one of our face-to-face courses will be given free access to the on-line course for one year. Due to the on-going pandemic and need for social distancing, we rarely have external places to offer as we did pre-2020, but you can still host a study day for yourself and your colleagues.
If your site is participating in the OptiBreech Trial, your free online training package has already been updated.
What if I have attended an in-person course in the past? Access to the Refresher Course is only available to those who have purchased and completed one of our on-line courses, beginning in 2021. All of our previous courses have been advertised with one year’s access to our Vimeo Library. Content is updated regularly, so our recent courses are significantly expanded, based on current research, compared to those of previous years. If you have completed the main course, the system will automatically consider you eligible to take the Refresher. If you use our videos for teaching within your institution, we encourage you to ask your employer to reimburse your training so you can continue to maintain access.
Finally, some opportunities to become more involved in Breech Birth Network. We would really like some help with the following, and if you are willing to make a regular commitment and develop the skills necessary, we can also pay you! Emma and I developed the skills to do all this because that is what was necessary, and we know others can too.
Ideally, we would like to involve people who are supporting breech births professionally in some way, so that the learning that occurs in these roles also spills over into developing your own practice. That’s what makes it worthwhile for us. And obvs, we expect that you would have completed our training to know what you are getting into and that your approach to breech birth aligns with ours.
If you are interested in any of these roles and prepared to make a commitment to helping our small, not-for-profit enterprise grow, please get in touch using the form below.

Round 1 of the international multi-stakeholder Delphi study, Development of a Core Outcome Set for Effectiveness Studies of Breech Birth at Term (Breech-COS) is now open. We invite the involvement of anyone from the following stakeholder groups, who has experience of care for women having vaginal breech births:

You can read more information about the research and participate using the link or the QR code below. You are welcome to share this post or forward to your stakeholder associates.
Participation Link: https://qualtrics.kcl.ac.uk/jfe/form/SV_b4uw2QJxcTC8oZM
This consensus-building activity follows on from our systematic review, including Patient and Public Involvement (PPI) activity, Development of a core outcome set for effectiveness studies of breech birth at term (Breech-COS): A systematic review on variations in outcome reporting.
Shawn Walker, on behalf of the OptiBreech team

My name is …, I’m a third year student midwife at X University and I am about to begin my literature review, I have decided to focus on vaginal breech birth. I haven’t finalised my question yet as I feel I need to read some more research to be able to word it correctly but I’m really interested in vaginal breech birth and practictoner skill. I’m ambitiously hoping my review might encourage the trust I work in to trial a breech birth team. I was wondering if you might be able to point me in the direction of any research regarding practitioner skill or breech birth teams? I understand we need much more research, but in your opinion is there any particular area that is really lacking in research that would support a move towards normalising vaginal breech births? I appreciate this is a very busy time for everyone having to work from home and understand you may not have time to respond to me at the moment but I’m so excited at the idea that don’t want to leave any stone unturned, any advice you have would be very appreciated.
Hope to hear from you soon!
(Thank you for permission to share this exchange.)

Hello,
Thank you for your message and your interest.
I write about this topic constantly https://breechbirth.org.uk/publications/. My PhD thesis contains a section on it, although this is a few years old now. Reference lists to our publications will help get you started. We also include information on building competence in the Breech Birth Network on-line training.
You could do a review on breech teams, breech clinics or midwife involvement in breech care. We need someone to lead some sort of consensus project to produce something like this for breech midwives: https://www.networks.nhs.uk/nhs-networks/diabetes-midwives/documents/NHSDAKC%20Midwives%20Standards.pdf That is a long-term project that will require funding, support and networking with key stakeholders, such as the RCM and RCOG. But it starts with a literature review.
You could do a literature review around midwives’ roles, any literature about competencies already out there, any evidence about the roles that midwives are taking, any evidence about outcomes associated with midwife-attended breech births (there is some in one of the TBT follow-up studies, I think by Su?).
My advice would be, whatever you do, treat it as a first step in becoming an expert in this area yourself. While it is great to try to convince your Trust they can do this, eventually, someone is going to need to actually put themselves on call and attend the births. So while you understandably feel at the beginning of a journey, see yourself as starting and committing to that journey, rather than trying to convince someone else to 😊 It may take years, but the breech revolution is a looooong-term game, requiring all of us to take small steps, with patience, but continuing to move forward, inch by inch. You will be constantly running into a wall. We turn to each other for support, do not give in to despair, and keep going. Eventually, enough of us running into the same wall will knock it down.
Another option is to do a review of outcomes associated with breech clinics and breech teams. This would be very valuable, but it will require a ‘no stone unturned’ approach indeed. This is because content about clinics and teams is usually embedded in articles, rather than listed as a key word. So you would have to do a general search on ‘breech presentation’ after 2000, eliminate obviously irrelevant articles and duplicates, then do searches on the words ‘team’, ‘clinic’ and ‘specialist’ and other related words such as ‘on-call’ and ‘stand-by,’ within the abstract and text of the articles themselves. It’s not as simple as a PICO search on randomised controlled trials, but it would pull together the general trends associated with clinics and teams (for ECV as well as VBB results), demonstrating a need for further research focusing on these as interventions themselves. (Here’s an example to get you started.)
To that end, make sure you are using a Reference Management Software programme. I use Mendeley. If you are going to become a breech specialist yourself, you will need to be very familiar with the literature and have it easy to hand when you want to apply for funding or write up your work. Do that now and begin to build your library of evidence, organised to help you make your arguments. Reference Management Software will also help you search the text.
Be sure to check the reference lists of any articles that qualify and our publications.
And choose a topic that you are interested in going on to do further research about because a literature review is the first step. Aim to write a literature review that you can publish, even in a student midwife journal, but ideally more. You are not doing a ‘student midwife literature review.’ You are doing a literature review. There’s no reason your first go need be any less worthy than any medical or post-graduate student doing a literature review for the first time, many of which get published. Your work and your mind are just as worthy, and when you spend time doing something properly, you have insight others can learn from.
Once you graduate, begin to identify sources of funding for the next stages. Research/breech practice is a great combination because it gives you some flexibility (e.g. not responsible for as many clinics/shifts) and helps move practice forward.
If you’ve done our on-line training, you can begin to become involved in assisting with training through BBN. Continual review and engagement is the best way to continually develop your confidence. We have on-line seminars frequently.
I am very happy to provide specific advice and guidance as an external supervisor for students who are intending to follow through, taking their project to publication. We need more voices contributing to this effort.
Best wishes,
Shawn
Update: I just undertook a mini literature review due to a student reporting how difficult it was to find qualifying papers. First: sympathy. Yes it is. Second: Unfortunately, there is no shortcut for very thorough understanding and overview of a topic in which you would like to gain expertise.
But how exciting! Every time I do this, I learn more, from discovering more qualifying papers to other topics that people have looked into. I could spend all day lost in these papers, connecting one to the other, piecing the jigsaw together. However, I need to get on with other things. First, some more tips: